“Like being rubbed with a cheese grater.”
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
That is how Bendigo woman Tara McGrath described the experience of getting dressed in the morning without medication for her fibromyalgia.
And while she takes more potent pain relief medications to cope with the chronic condition, a sudden flare up of symptoms could sometimes be eased with the help of over-the-counter codeine tablets.
“Taking that would be the difference between being able to function through my flare, or not,” she said, describing the fatigue and muscle soreness that could besiege her body.
“That's not a thing I would be able to do now, unless I can get my GP to prescribe for me.”
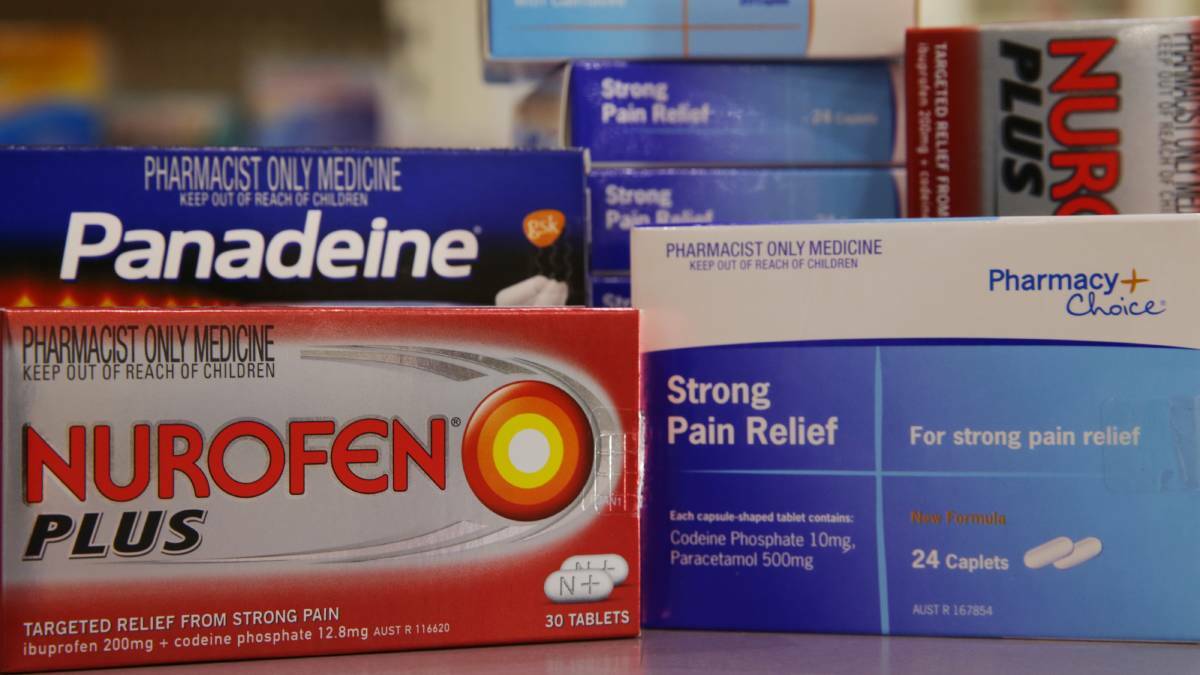
A Therapeutic Goods Administration reclassification of low-level codeine products like Nurofen Plus and Panadeine came into effect on Thursday, meaning users can no longer access the drugs without first obtaining a prescription.
The move seeks to reduce the rate of opioid-related addiction and death in Australia.
There were 372 recorded overdose deaths from pharmaceutical medicines in Victoria during 2016, more than illegal drug overdose deaths or the state’s road toll.
But Ms McGrath pondered what the change would mean for people unable to access the medication on which they once relied.
She anticipated seeing her general practitioner would become more difficult now codeine users were also seeking appointments.
“I worry also it’ll lead to more deaths, rather than less, because people previously using codeine will, instead of going to doctor, say, 'I'll go onto the synthetic weed', or something worse,” she said.
“If you’re in enormous amounts of pain, you don’t think your actions through.”
La Trobe University clinical pharmacy lecturer Pene Wood said it was not yet clear what would change after February 1 for people living in chronic pain.
Pain has such a big cost on the community and the healthcare system if it's not managed properly because it goes along with depression and mental health issues that can be problematic as well.
- Pene Wood, La Trobe University clinical pharmacy lecturer
It was possible some who no longer had easy access to codeine medication could experience opioid withdrawal, the symptoms of which included: aches and pains; an upset stomach; irritability and an inability to sleep.
“They may not even know what they're going through, just feeling lousy,” she said.
The lecturer expected some people with addictions would need medication to wean themselves off the drug.
But she supported the change to the drugs’ classification, saying they were not appropriate for long term use and were instead better to combat acute pain, or flares of chronic plain.
Other pain management options were available and pharmacists were able to counsel their patients on what would suit them best, Ms Wood said.
Many had spent the past six months preparing for the change and were well equipped to offer advice.
“It is also important to remember that a little bit of pain is okay, it's your body protecting itself from damage,” Ms Wood said, while also adding that it was important to be empathetic towards people living with pain.

It was an at times debilitating condition, she said.
“Pain has such a big cost on the community and the healthcare system if its not managed properly because it goes along with depression and mental health issues that can be problematic as well.”
Her view was backed up by the dozens of medical authorities around Australia also in support of the over-the-counter ban, including the colleges of physicians and GPs, as well as peak body Pain Australia.
It’s chief executive, Carol Bennett, suggested physiotherapy, daily exercise, behavioural changes and cognitive behavioural therapy as alternative pain management strategies.
“It’s important that people living with chronic pain are given all the options and are supported by their clinicians to be able to access the treatment that’s most appropriate for them.,” Ms Bennett said.
“Often it isn’t simply a tablet.”
The codeine move was not an unusual one either, with 25 other countries already requiring a script before codeine can be sold.
Seeking help from a pharmacist was a step Ms McGrath supported, in theory. In fact, it was a community pharmacist who first helped diagnose her fibromyalgia.
“But it depends entirely on the pharmacist you get, and their level of understanding,” she said, recalling had less satisfactory experiences at a chemist after which she walked away feeling condescended to.
“It's just a case of lessening (the pain) enough so we can function,” Ms McGrath said.
“We're not trying to be Olympic athletes.
“We just want to hold down a job.”


