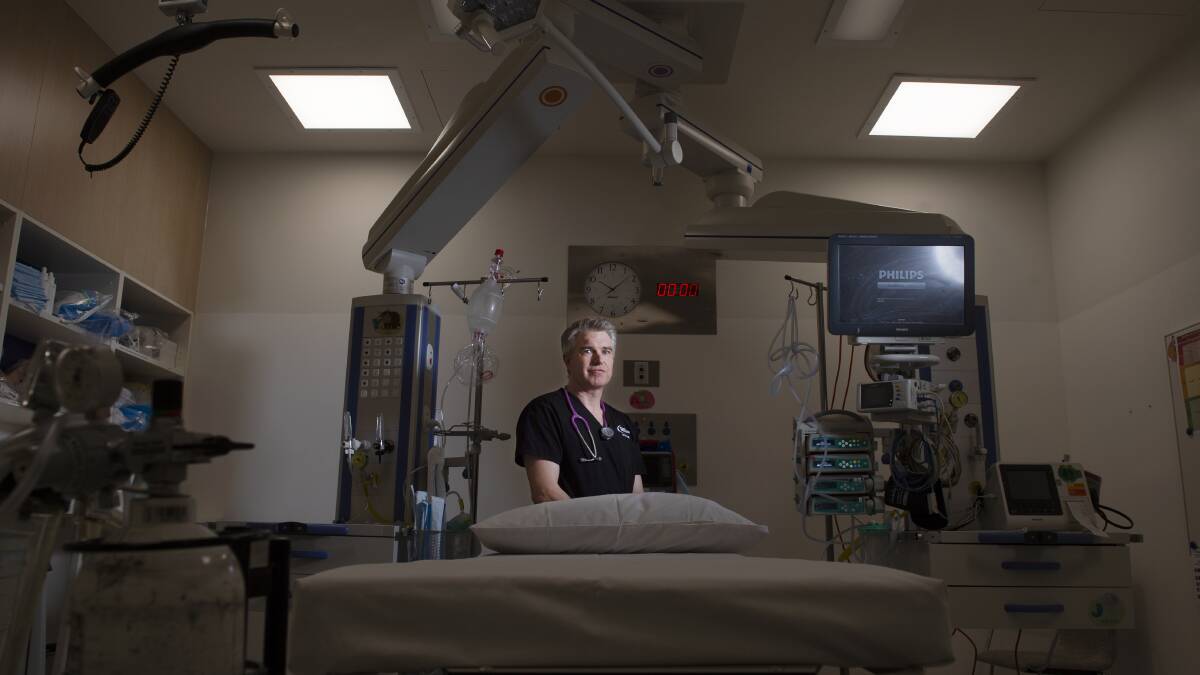
"We were preparing to be inundated and to have huge number of patients."
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
Bendigo Health workers have experienced a start to the year like none before as they prepared to fight a deadly pandemic.
As the novel coronavirus spread from China, doctors, nurses, and other health workers, put aside fear of the unknown to prepare to save lives in Bendigo.
At one point staff expected a situation like in New York or Italy: to be inundated with COVID-19 patients, for the system to be stretched to its maximum.
Staff talked about putting patients in bunks, treating people in corridors, even at worst, a military style triage.
Now the hospital has a separated emergency department. It can funnel risky patients through a separate system, with separate corridors.
Changes that would normally take months have been made in weeks.
It's taken 21 hour days and weeks of heavy overtime from hospital staff.
Health workers have also been on an emotional journey, preparing for risks to themselves and their families.
Facing the unknown
The first reports of a new coronavirus came out of China in late December.
It wasn't until Australia Day that Bendigo's hospital began to see its first suspected cases. These were people who had travelled to high risk areas, at that stage China.

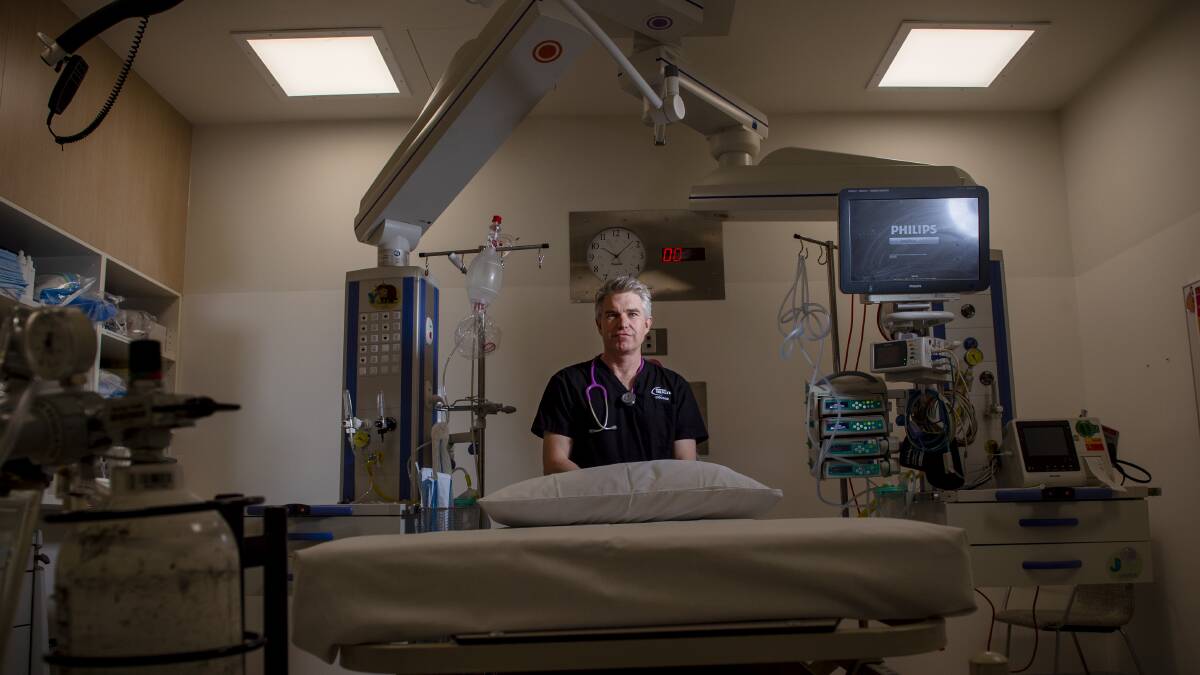
Clinical director of acute and ambulatory care Ben McKenzie said doctors knew very little about the illness then.
"We sort of new it would be similar to SARS or MERS ... but we had really limited information about how widespread it was, how deadly it was going to be, and how many people were going to get really sick," Dr McKenzie said.
Hospital staff expected to to treat huge numbers of COVID-19 cases when Australia first began to see the coronavirus, he said.
Staff were meeting daily about ventilators, and discussing spaces to look after patients needing respiratory support.
"We knew it was going to come to Bendigo eventually. And we were prepared for suspected cases. And then we were prepared for confirmed cases," Dr McKenzie said.
"Then we were preparing to be inundated and to have huge number of patients."
Dr McKenzie said reports of disaster unfolding in Italy created a sense of urgency among the staff. There was fear about what could happen in central Victoria.
He said it was hard for staff, who knew the virus could affect them personally, their colleagues, patients and families.
Am I going to die from this?', is a question that everyone's asked themselves.
- Doctor Ben McKenzie
"When you're there, and you've got your personal protective equipment on, and you've got your hands on a coronavirus patient, and you've got to treat them, that becomes difficult because your own health is definitely at risk," Dr McKenzie said.
"'Am I going to die from this?', is a question that everyone's asked themselves."
But Dr McKenzie said the proactive approach to minimising risk from hospital leadership helped staff navigate this.
Bendigo Health acting director of clinical operations Carol-Anne Lever said she felt a sense of urgency about preparation.
It came as Mrs Lever saw how "horrendous" the situation could be, from reports on the internet.
There was a "real sense of impending doom", she said.
Information was coming from everywhere, Mrs Lever said. But it was hard to know how quickly the situation would escalate.
"It was really about sitting down with the teams and saying, 'What are we going to do here? Where are we going to start?" she said.
Pandemic proofing
Staff began at the hospital's front door.
They split the emergency department, essentially creating two systems. A nurse separated possible COVID-19 patients from others before they even walked in the door.
Director of infection control Jane Hellsten said Bendigo Health was quick to form a pandemic planning team, which started with an outbreak management plan.
It soon became obvious that this was bigger than any management they had been involved with in the past, she said.
In the news Mrs Hellsten could see the virus overwhelming the healthcare system of Wuhan.
She said the feeling was similar to the 2002 SARS outbreak: a fear of the unknown. Health workers did not yet know how the virus would behave, its infectiousness, or its mortality rate.
"What was coming out of China didn't look good, or sound good. It seemed to be highly infections, easily transmitted, and a serious virus," she said.
"It was causing high mortality rates in China. It was scary. I think we were on high alert."
Key people on the team split into groups to take on specific tasks, covering different aspects of the pandemic planning.
It mean training staff, making sure they had necessary equipment, having safety apparel, ensuring everybody was aware of processes, from triage to ED, to intensive care.

This training has been ongoing.
Personal protective equipment soon proved a key aspect of the preparations.
Shortages were a problem world wide during March and April.
Unable to rely on disposable PPE supplies, Bendigo Health staff were forced to think creatively about how they managed the equipment.
This has meant locally manufactured visors, launderable gowns, and "phenomenal" help from local industry.
"Early on I think everybody realised everywhere that there wasn't necessarily going to be adequate PPE," Mrs Hellsten said.
"We had to also look at alternatives and novel ways of getting PPE for healthcare workers."
Even the hospital's design played in to preparations.
Opened in 2017, the facility was planned in the aftermath of the 2009 Swine Flu.
Dr McKenzie said this meant Bendigo had one of the best set ups in the state, even in Australia, to isolate patients for a pandemic.
Mrs Lever said Bendigo was lucky to have the physical space to take steps like splitting its emergency department.

As a regional centre, it also had 12 beds for patients in case of a pandemic.
But if it came to it, this "would have done jack dandy", Mrs Lever said.
It did mean the hospital could funnel people through a different area, to keep them separate, she said.
The hospital put in place separate hallways, separate corridors. Negative pressure systems could even keep air in certain spaces isolated.
Mrs Lever said staff talked about putting people in bunks or corridors, as they expected hundreds of patients.
Hearing stories from Italy, they faced the prospect of some not even making it in to the emergency department.
As clinicians - with the first instinct to treat people - it was a struggle, Mrs Lever said.
"Part of our disaster planning is when we get worst, worst case scenario, we had basically a field triage," she said.
"We literally got down to that level of planning where we had to face the prospect that we might not be able to treat everyone."
For Dr McKenzie, it was a very different experience from planning for previous coronavirus outbreaks such as SARS in 2002.
Clinicians could share experiences rapidly using emails. Within hours healthcare professionals could use information about something that had happened elsewhere, be it Victoria, Australia or overseas.
Were we ready? Yes, we were ready. We knew what to do.
- Jane Hellsten
That Bendigo Health doctors understood early how COVID-19 was likely to progress in patients was key.
Dr McKenzie said this meant doctors could plan well when they identified a coronavirus patient.
"When we had our first number of cases we understood what was likely to happen to them, and when they were likely to deteriorate," Dr McKenzie said.
"We didn't have to make all our own mistakes. We were able to use all of the information available to provide best care for patients, even though we'd never seen this new disease before."
Ready for COVID
Even with heavy preparation, the first coronavirus case was going to be a shock, Mrs Hellsten said.
"You think 'Crikey, we've got somebody who's positive for COVID-19'. The alarm bells will still go out," she said.
"Were we ready? Yes, we were ready. We knew what to do."
The hospital had done an "awful lot of planning" to get to that point.
Mrs Hellsten attributed Bendigo's readiness to a strong executive team, following guidance provided by the Department of Health and Human Services.
And from her position, Mrs Lever has been amazed by the willingness of staff to adapt to the sheer amount of change.
The hospital's workers have been "amazing" during the crisis, she said. She saw resilience and passion from teams at Bendigo Health as they faced change.
'Stay vigilant'
With every week, Bendigo Health is starting to turn more of its normal operations back on.
But Mrs Lever said some aspects of the hospital's operations will never go back to the way they were. For instance, it's allowing visitors, but still screening patients for respiratory conditions.
Mrs Lever said the hospital would have to maintain all its systems and extra staffing until the coronavirus was eliminated. She said health workers knew they would see spikes, some of them in Bendigo for sure.
"We're still all very cautious waiting for something to happen still," she said.
"We're not out of this until we've got a vaccine."
And in the back of her mind, Mrs Lever knows winter is coming. Every year the season brings respiratory illness, and worsens existing asthma and emphysema.
If COVID-19 came with winter, it would be a real worry, she said.
Likewise, Mrs Hellsten warned central Victorians to stay vigilant.
She said the hospital's COVID-19 tests were throwing up results for other viruses, such as the common cold.
"The need for hand hygiene and respiratory hygiene and social distancing, it's still real, it's still needed," Mrs Hellsten said.
"We're heading into winter. Our fear is we're already seeing an increase in cold viruses, so we expect to see an increase in the spread of flu, in colds, and potentially COVID-19.
"Stay vigilant. Don't think that it's over. It's not."
Dr McKenzie said Bendigo Health staff were still trying to make sure people were safe, even with low case numbers in Victoria.
He has seen staff make an emotional journey, and been proud of the result.
"We have an incredibly strong group of people who are willing to rise to the table. We feel like we can really respond to anything now we've prepared to this level," Dr McKenzie said.
"We're all incredibly proud of all the staff who have stepped up managing patients with coronavirus who need their care and are incredibly sick. The staff have done a really great job."
Have you signed up to the Bendigo Advertiser's daily newsletter and breaking news emails? You can register below and make sure you are up to date with everything that's happening in central Victoria.


