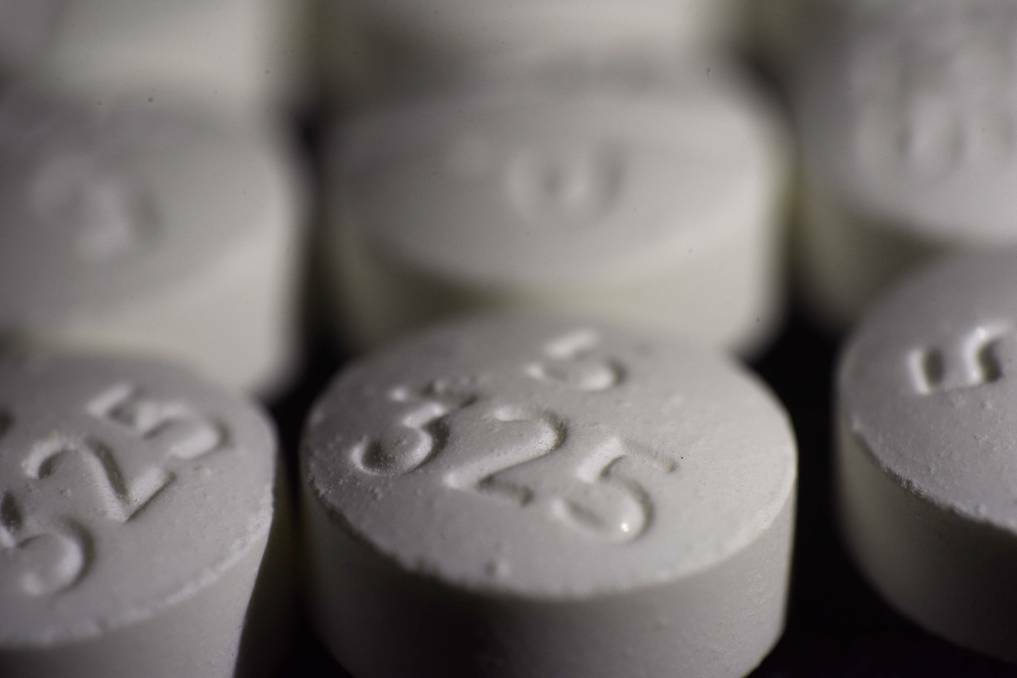
Patients need better support in a health system grappling with an 87 per cent spike in prescription opioid deaths.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
GPs are struggling to find specialist care services for patients outside of the hospital system, Bendigo Community Health Services’ Graem Kelly said.
While hospitals provide drug withdrawal services, patients need specialist clinics as general practitioners take greater responsibility for tackling addiction for medication, he said.
Prescription opioid deaths shot up 87 per cent between 2008 and 2014, according to a 2018 Penington Institute report.
The medications were the most fatal drug type in Bendigo from 2001 to 2016.
Clinics need the capability to provide patients with care across specialties, Mr Kelly said, including physiotherapy, exercise physiology, counselling, specialist GP and drug management services.
“Patients’ needs can become quite complex and Medicare does not respond well to that sort of treatment,” he said.
“So there is a place for both state and federal governments to look at that at the primary care level.”
La Trobe University pain management expert Pene Wood said prescription medication was a particular issue in regional areas, where chronic pain sufferers could struggle to find multidisciplinary support services.
“People suffering from chronic pain need to understand that medication alone is not the answer – and that health professionals can help them put alternative strategies in place,” she said.
Those strategies, combined with public education campaigns, were increasingly important in the lead up to this year’s SafeScript rollout, Ms Wood said.
The software was designed to help healthcare professionals track prescriptions and Ms Wood said it would likely make doctors more reluctant to prescribe main management medication.
A SafeScript pilot program had already identified people who could benefit from alternate treatments, Ms Wood said, but doctors were often unsure what to do with those patients.
“So I think having more awareness about appropriate pain management is important for doctors and for consumers,” she said.
Mr Kelly said GPs’ prescriptions were already being more closely monitored than in the past.
“And let’s face it, there is probably a growing awareness by GPs and their patients of these issues. They don’t want to be dependent and beholden to these drugs,” he said.
Exercise could be key to pain treatment
Exercise may be the weapon many relying on addictive pain medication are yet to discover, a Bendigo researcher says.
La Trobe University’s Pene Wood is part of a group preparing to cycle 700km over eight days in Tasmania for the Pain Revolution Rural Outreach Ride.
The event will take place in March, with riders educating people in communities they cycle through and raising funds to supply local pain educators.
“I’m a pharmacist and I’ve seen first hand where people have relied on medication to manage pain and run into trouble with dependence,” Ms Wood said.
“I want to help educate people and to prevent that.”
Messages about the importance of exercise and other treatments were still to resonate with many people using prescription medication.
“People are still fearful of doing exercise. they are concerned if there is pain they are going to make it worse, which is actually not true,” she said.

“I think it’s really important to get that message out there.”
Footscray exercise physiologist Brendan Mouatt said people interested in coming off medication and replacing it with exercise should consult a medical professional.
“However, with exercise, especially through research, we see even small amounts of exercise can be really beneficial in tapping into our natural opioid and pain killing systems,” he said.
While people who had not exercised in a while could experience discomfort, pain did not always equate to damage, Mr Mouatt said.
“So sometimes having guidance from someone like an exercise physiologist can be really helpful initially,” he said.
Getting started could be the hardest part. Mr Mouatt said people experiencing chronic pain tended to move less than those who had no health issues.
Bendigo Community Health Services executive director Callum Wright said that as people stepped down from opioid addiction they needed physiotherapy or exercise physiology therapies to help them manage withdrawal and pain management.
Mr Mouatt said exercise could help people improve their capacity to move as well as to strengthen their mental health and social interaction.
“And in a way it gives you something you can control,” he said.
“Often good exercise prescription can be a way for us to even control pain, which is something opioids don’t give us. We are reliant on an external means.”
To find out more or donate to the Pain Revolution Rural Outreach Ride visit www.painrevolution.org
Have you signed up to the Bendigo Advertiser's daily newsletter and breaking news emails? You can register below and make sure you are up to date with everything that's happening in central Victoria.


